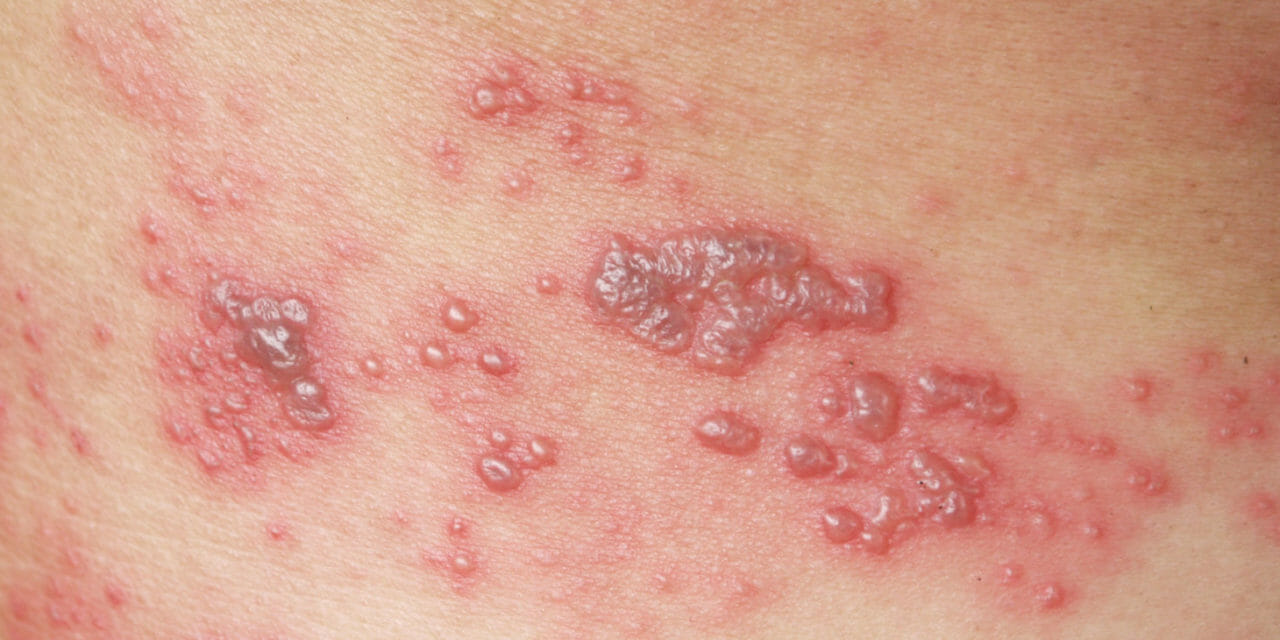
At 26 years old and pregnant, my mom broke out with red, itchy, blister-like spots and patches primarily on her torso and back.
Her physician, a family medicine doctor in a small town of less than 500 people in rural South Dakota diagnosed with her German or “hard” measles, maybe chickenpox, or perhaps something called shingles. Each of those maladies had similar characteristics.
“We had never really heard of shingles back then or knew much about them,” Uken said.
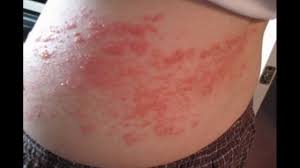
It was the mid-1960s.
He prescribed some ointment to help with the itch and sent her home pregnant and in agony. There was nothing more seemingly he could do.
At age 74, upon her daughter’s advice, Uken got a shingles vaccine.
“So many at her workplace were getting the shingles she scared us,” Uken said. Both she and her husband got the vaccine.
She knew that even if what she had decades earlier was indeed shingles, she could get them again. She had no desire to live through that pain again.
Four years after receiving the vaccine, Uken got shingles. They were located on half of her stomach, over her hip and back to her spine. They lasted about six weeks.
They were not, she said, as bad as perhaps they could have been and believes the vaccine helped.
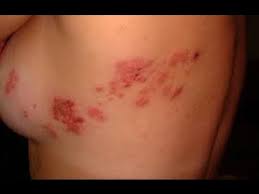
At least 1 million people a year in the United States get shingles, a painful and often debilitating skin rash, often with blisters, according to the Centers for Disease Control and Prevention.
Anyone who has ever had chicken pox can get shingles (herpes zoster), a painful rash that arises on one side of the face or body that can cause blisters and scabs and can take weeks to resolve. But a vaccine (Zostavax) can cut your chances of that.
What causes shingles?
Shingles is caused by the varicella-zoster virus, which remains dormant in the body long after the last chicken pox has faded. It can become active again decades later in the form of shingles.
The most common complication of shingles is postherpetic neuralgia (PHN), which causes severe and sometimes debilitating pain in the rash area and can last weeks or months—and occasionally years—after the rash has cleared. Other serious complications include vision loss, pneumonia, or inflammation of the brain (encephalitis).
Symptoms
The main symptom of shingles is pain which can be severe, according to the Washington State Department of Health. About one in five people experience severe pain that continues even after the rash clears up. Other symptoms of shingles can include:
· Fever
· Headache
· Chills
· Upset Stomach
What about the vaccine?
Although not guaranteed to prevent the development of shingles, the vaccine reduces your risk by 51 percent, according to the Centers for Disease Control and Prevention, and cuts the risk of PHN by 67 percent. The vaccine costs about $220 so check with your insurance carrier to see if it will help cover the cost.
Here’s what else you need to know about Zostavax:
• The CDC recommends the vaccine for most adults ages 60 and older—even those who have already had a bout of shingles—and some experts feel that people in their 50s should be vaccinated as well. People vaccinated against shingles at a younger age (for instance, in their 50s as opposed to their 60s) may face the possibility of developing shingles later in life once the vaccine is no longer effective—and when complications from shingles may be more severe.
• Zostavax is most effective for the first five years, although there may still be modest protective benefits for a few years after that.
• Currently, there is no recommendation to administer booster shots to people; it’s therefore important to discuss any risk factors or concerns with your doctor about the timing of your vaccination.
• If you don’t recall having chicken pox as a child, you should still get the shingles vaccine. More than 99 percent of people over 40 suffered through chicken pox as young children, expert say, so chances are you did have the disease. If you never had chicken pox, getting the Zostavax shingles vaccine will do no harm to you. In fact, even if you’ve had shingles before, the vaccine could help prevent a new case of it.
• People who shouldn’t get the vaccine include those who are allergic to gelatin, the antibiotic neomycin or any other component of the shingles vaccine; have a condition that weakens their immune system, such as HIV, leukemia or lymphoma; are undergoing cancer treatment; are using high-dose corticosteroids; or may be pregnant.
• Medicare Part D covers the vaccine, under the pharmacy benefit. To assure reimbursement, get your vaccination from a pharmacy instead of your doctor.
This article first appeared on HealthCentral..com.